The Evidence-Based Nursing Unit
The Evidence-Based Nursing Unit (EBNU) exists to drive and support our nurses in translating evidence into practice and provide support to nurses in conducting systematic review and primary research. The unit support nurses with the preparation of research proposals, grants and Institutional Review Board applications. We also provide research/Evidence-Based Practice (EBP) trainings that will have impact on practice issues, governance and policy.

About Us
Our milestones
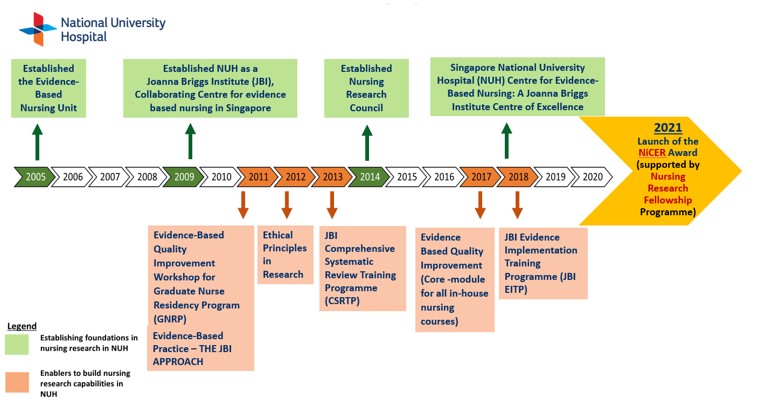
The EBNU was established in May 2005 with the objective of building the capability and capacity of nurses to adopt best practice standards. The EBNU was officially launched in 2008. Over the years, the unit has progressively fulfilled its mission of creating awareness and promoting evidence-based practice amongst our nurses.

In 2009, the signing of the Memorandum of Understanding between NUH, Evidence-based Nursing centre and JBI (Adelaide) took place in Singapore. Since then, NUH Nursing department embarked on the journey towards EBP together with more than 75 Collaborating Entities across 40 countries to improve the quality and healthcare outcomes. In 2014, we affirmed our presence as an EBN Centre of Excellence by hosting for the first time
the 9th Biennial JBI Colloquium in Singapore.
THE Nursing Innovation, Clinical Inquiry, Enabling Research (NiCER) AWARD
Conducting and translating research is embedded within our vision and mission as an Academic Tertiary Hospital at NUHS, where research forms one of the pillars for delivering quality care to our patients. The NiCER awards was launced in 2021. Our long term vision is to nurture and build capability of our nurses in conducting nursing research and driving evidence-based care at NUH.
Click
here for more information of the award and awardees.
Advanced Practice Nurse
NUH has a group of Advanced Practice Nurses (APNs) who are well-equipped with a wide knowledge base, complex decision-making skills and clinical competencies for extended practice. Trained in the diagnosis and management of common medical conditions including chronic illness, they work independently and in hand with the doctors and other healthcare professionals to provide complex care to patients.
Our specialties include:
Critical Care | Diabetes Care | Emergency Care | Geriatric Care | Mental Health |
Midwifery | Neonatology | Nephrology | Neuroscience | Oncology |
Orthopaedic | Paediatrics
| Palliative Care | Organ Transplantation
| |
Advanced Practice Nurse Council
The NUH Advanced Practice Nurse (APN) Council aims to shape the development of APNs and contribute towards an academic practice environment at National University Health System through clinical excellence, leadership, education, consultation, and research. We strive towards this by working on the following:
1. Design and develop the role of APNs in delivery of healthcare services across a variety of clinical settings.
2. Encourage interdisciplinary collaboration among APNs, within and beyond NUH.
3. Promote and lead the development of research, evidence-based practice and outcomes evaluation related to APN practice.
4. Nurture the next generation of nurses towards advanced practice nursing to meeting the ever-changing healthcare needs.
5. Represent NUH on issues relating to APN practice at various national and international healthcare platforms.
The APN Journey, Shared by Cindy Chua

"I started out as a young and aspiring nurse working in the Surgical General Ward since 1998. Three years later, I pursued my Advanced Diploma in Nursing (Medical-Surgical) and was posted to the Intensive Care Unit (ICU) upon my graduation. Since then, I stayed on and never looked back. I love the challenges and excitement that the ICU settings brings. I went on to attain my Bachelor’s degree at University of Sydney and Master’s degree (Advanced Practice Nurse) at the National University of Singapore (NUS). I have been a full-fledged APN since 2010."
Click
here for APN Cindy's journey of becoming an APN.
Back to Top