This treatment involves the placement of a small probe about the size of an injection needle into the thyroid nodule. Thereafter, the tip of the probe is activated, and this creates a radiofrequency wave that essentially heats up the nodule, thereby destroying the cells within the nodule.
This procedure may be performed under sedation, local or general anaesthesia. Local anaesthesia and sedation are preferred, to allow better monitoring of patients. The procedure lasts for 30-45 minutes depending on the size of nodule for ablation.
Local anaesthesia is administered in the neck to ensure there is minimal pain and discomfort during the procedure. Following this, cold fluid may be injected around the thyroid to prevent heat transmission to the surrounding structures. Thereafter, the RFA probe is inserted into the thyroid nodule under ultrasound guidance and the probe is activated to allow for thermal ablation of the nodule.
How RFA procedure is done:
| 
|
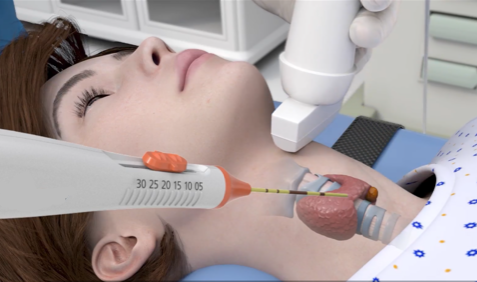
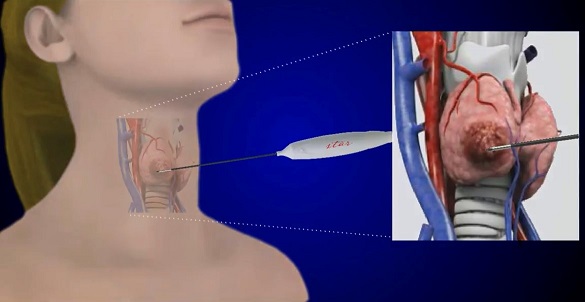
Radiofrequency ablation (RFA) procedure - a small probe is inserted into the thyroid nodule. This may be done under local or general anaesthesia, or sedation. Patients typically experience minimal discomfort during and after the procedure.
Activated RFA probe in the thyroid nodule:
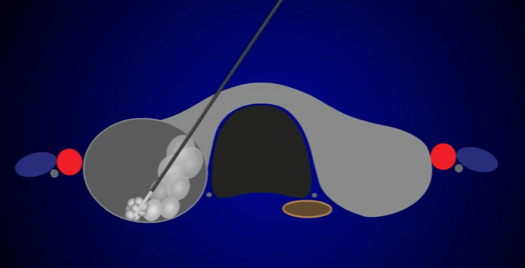
RFA probe being activated in the thyroid nodule - leading to thermal destruction of nodule with preservation of surrounding thyroid tissue.