Associate Professor Tan Ker Kan
Head of Division
Senior Consultant
A/Prof Tan specialises in both minimally invasive procedures for primary and recurrent colorectal cancer and complex colorectal conditions, with a keen interest in proctology work especially in anal fistula and haemorrhoids.
Specialties: Colorectal Surgery, Surgical Oncology (Colorectal Surgery)
Clinical Interest: Colorectal cancer, Keyhole/Laparoscopic surgery, Anal fistula, Haemorrhoids, Anal fissure, Colonoscopy, Recurrent colon and rectal cancer, Colorectal polyps
Languages Spoken: English, Mandarin, Hokkien, Malay (simple)
View Profile Make an Appointment

Adjunct Associate Professor Cheong Wai Kit
Senior Consultant
Adj Assoc Prof Cheong has vast experience in the management of diseases of the colon, rectum and anal canal, with special interest in advanced and recurrent colorectal cancer, abdominal and pelvic sarcoma, peritoneal cancer, and complex anal fistula.
Specialties: Colorectal Surgery, Surgical Oncology (Colorectal Surgery)
Clinical Interest: Minimally Invasive Colorectal Surgery, Recurrent and Advanced Colorectal Cancer, Pelvic Exenteration, Peritoneal Cancer, Abdominal and Pelvic Sarcoma, Complex Anal Fistula
Languages Spoken: English, Mandarin, Malay, Cantonese
View Profile Make an Appointment

Adjunct Associate Professor Bettina Lieske
Senior Consultant
Adj Assoc Prof Bettina specialises in peritoneal malignancies, with extensive experience in cytoreductive surgery and heated intra-peritoneal chemotherapy. She is dedicated to providing personalised care and achieving the best possible outcomes for her patients.
Specialties: Colorectal Surgery, Surgical Oncology, Surgical Oncology (Colorectal Surgery)
Clinical Interest: Diagnostic and Therapeutic Endoscopy (Gastroscopy and Colonoscopy), Laparoscopic Surgery for Colorectal Cancer and Benign Colorectal Conditions, Malignant Peritoneal Disease (Including Neoplasms of the Appendix & Pseudomyxoma Peritonei), Cytoreductive Surgery and Heated Intraperitoneal Chemotherapy (CRS and HIPEC), Pressurised Intraperitoneal Aerosolised Chemotherapy (PIPAC)
Languages Spoken: English, German
View Profile Make an Appointment

Adjunct Associate Professor Ian Tan
Consultant
Adj Assoc Prof Tan specialises in advanced laparoscopic (key-hole) colorectal surgery for cancer as well as inflammatory bowel disease. In addition to being an advanced endoscopist (colonoscopy and gastroscopy), he also specializes in the management of haemorrhoids, anal fistula and anal fissures.
Specialties: Colorectal Surgery
Clinical Interest: Colorectal Cancer, Diagnostic and Therapeutic Endoscopy (Gastroscopy and Colonoscopy), Minimally Invasive Surgery, Inflammatory Bowel Disease (Ulcerative Colitis and Crohn's Disease)
Languages Spoken: English, Mandarin, Malay
View Profile Make an Appointment

Adjunct Assistant Professor Norman Lin
Consultant
Adj Asst Prof Lin is a Colorectal and Trauma Surgery specialist with expertise in minimally invasive robotic and laparoscopic surgical techniques for colorectal cancer treatment, offering comprehensive care for colorectal conditions and traumatic injuries.
Specialties: Colorectal Surgery, Trauma Surgery
Clinical Interest: Colorectal Cancer, Laparoscopic Colorectal Surgery, Robotic Colorectal Surgery, Colonoscopy, Haemorrhoids/Piles, Anal Fistula
Languages Spoken: English, Mandarin, Hokkien, Malay (simple)
View Profile Make an Appointment

Adjunct Assistant Professor Dedrick Chan
Consultant
Adj Asst Prof Chan is an established colorectal surgeon with extensive experience. His clinical focus is on colorectal cancer and he delivers surgical care aimed at improving cancer outcomes.
Specialties: Colorectal Surgery
Clinical Interest: Colorectal Cancer, Laparoscopic Surgery, Minimally Invasive Techniques, Haemorrhoids/Piles, Anal Fistula, Advanced Colonoscopy
Languages Spoken: English, Mandarin, French
View Profile Make an Appointment
Adjunct Assistant Professor Lee Kai Yin
Consultant
Adj Asst Lee specialises in minimally invasive robotic and laparoscopic techniques for colorectal cancer treatment, with expertise in surgery, research, and medical education.
Specialties: Colorectal Surgery, Surgical Oncology (Colorectal Surgery)
Clinical Interest: Colorectal Cancer, Minimally Invasive/Robotic Surgery, Colonoscopy, Haemorrhoids
Languages Spoken: English, Mandarin
View Profile Make an Appointment
Dr Bryan Buan Jun Liang
Consultant
Dr Buan specialises in minimally invasive techniques and colorectal cancer treatment, with a strong focus on early detection and patient education.
Specialties: Colorectal Surgery, Surgical Oncology (Colorectal Surgery)
Clinical Interest: Colorectal Cancer, Minimally Invasive Surgery, Diagnostic and Therapeutic Endoscopy, Haemorrhoids. Anal Fistulas
Languages Spoken: English, Mandarin
View Profile
Make an Appointment

Dr Jarrod Tan Kah Hwee
Consultant
Dr Tan specializes in colorectal surgery, with advanced expertise in minimally invasive techniques and the management of recurrent or advanced colorectal cancers and abdominopelvic sarcomas.
Specialties: Colorectal Surgery, Surgical Oncology (Colorectal Surgery), Minimally Invasive Surgery
Clinical Interest: Minimally Invasive Colorectal Surgery, Recurrent and Advanced Colorectal Cancer, Pelvic Exenteration, Peritoneal Cancer, Abdominal and Pelvic Sarcoma, Complex Anal Fistula
Languages Spoken: English, Mandarin & Hokkien
View Profile
Make an Appointment
Dr Lim Tian Zhi
Associate Consultant
Dr Lim is committed to public health education with a focus on colorectal cancer screening and its associated health services.
Clinical Interest: Colorectal Cancer Screening, Public Health
Languages Spoken: English, Mandarin, Hokkien
View Profile
Make an Appointment


















.png)




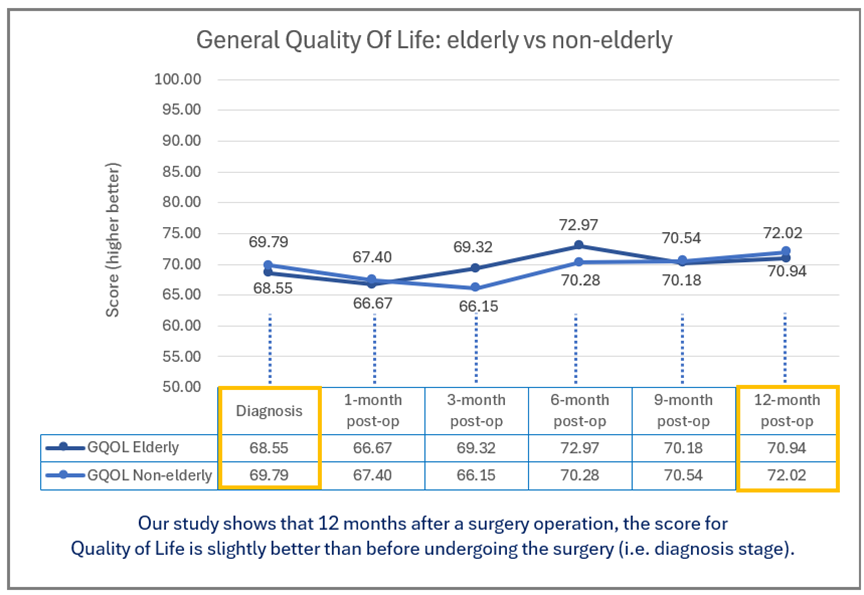
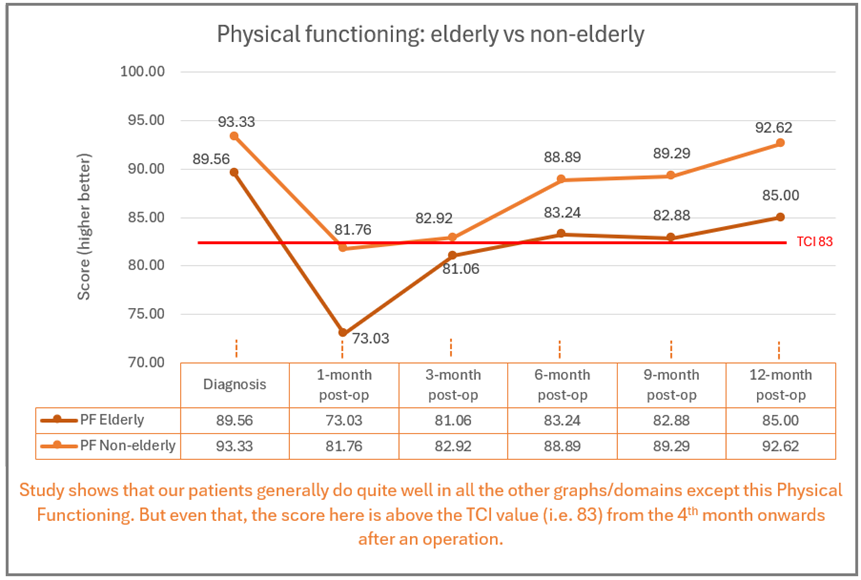
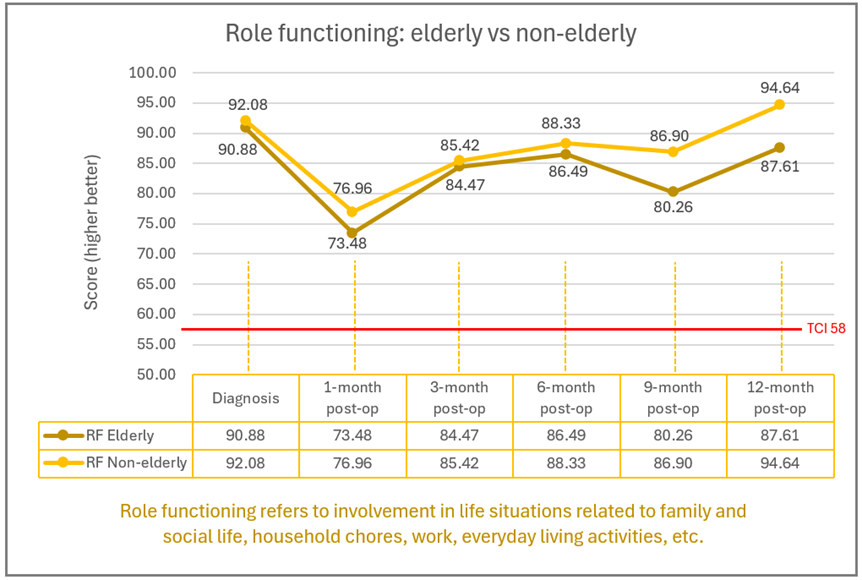
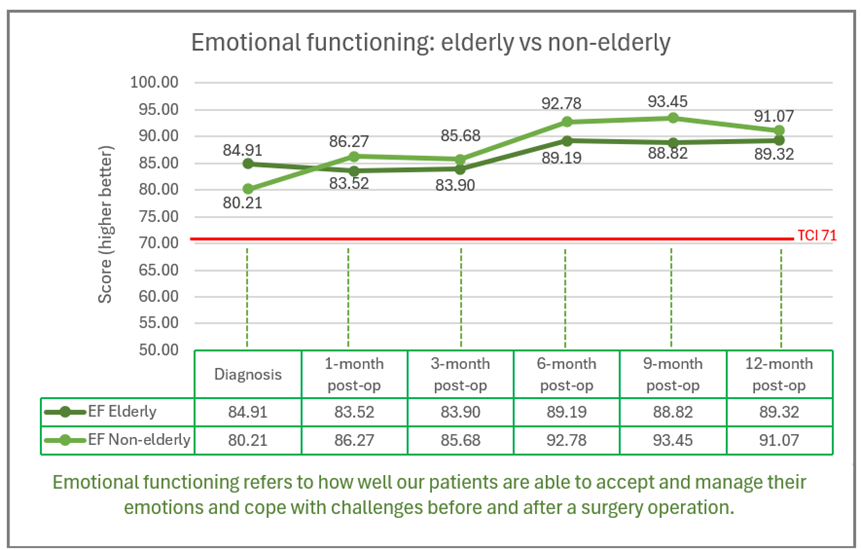






-edited.png)

-edited.png)


















