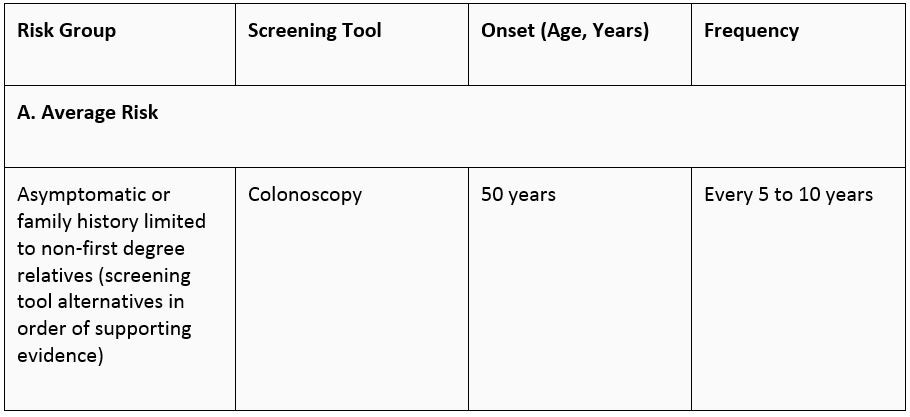
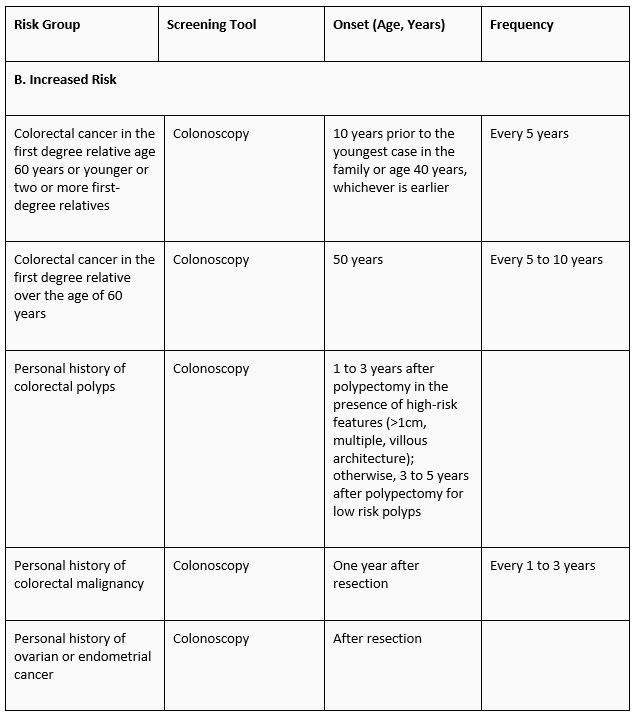
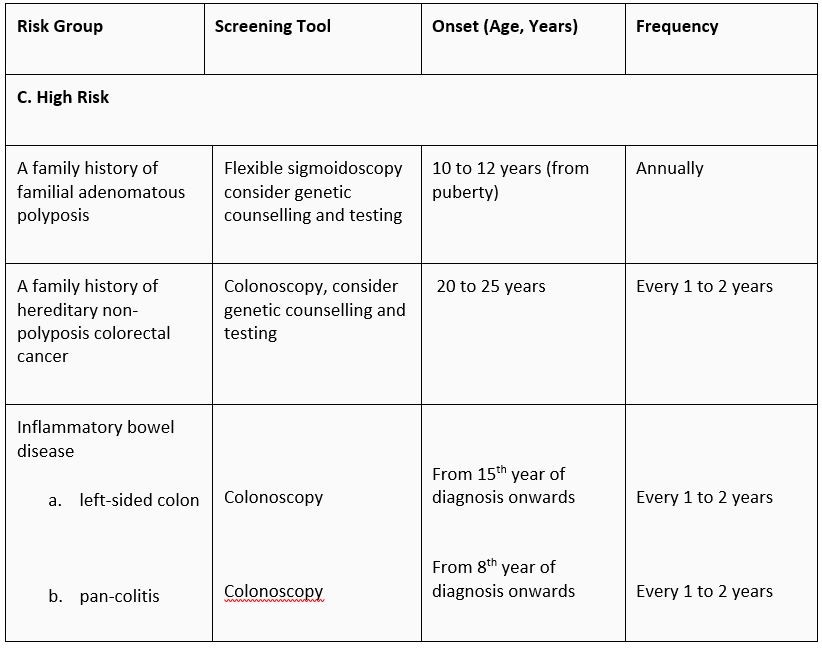
For a screening test to be widely applicable, it must be inexpensive, reliable and acceptable. Various screening tests for colorectal cancer have been reported. Faecal occult blood testing (FOBT) is the only screening modality that has been shown in three large randomised trials to show a 33% reduction in colorectal cancer mortality. In light of this, it would be almost medically negligent not to offer FOBT screening for average-risk individuals age 50 and above. The other commonly employed screening test is colonoscopy.
Other screening alternatives include barium enema, sigmoidoscopy and CT colonography (virtual colonoscopy). However, current evidence suggests that these alternatives may not be as effective and reliable as FOBT or colonoscopy in large-scale population screening.
Faecal Occult Blood Tests (FOBT)
Immunochemical FOBTs detect human haemoglobin from partially digested blood in the stool. They are more sensitive and more specific than guaiac-based tests that were used in the past. Another advantage is that dietary restriction is not required in immunochemical testing.
Further evaluation will be recommended if any of the two stool samples provided by the patient is positive. In a large UK study, 12% and 23% of FOBT-positive individuals had cancer and adenomatous polyps respectively on colonoscopy. Cancers detected at screening were of an earlier stage than symptomatic ones (Duke's A: 26% screened vs 11% in controls).
Immunochemical FOBT
The main disadvantage of FOBT screening is its low sensitivity. An estimated 50% of cancers will be missed on each screening round. To enhance the pick-up rate, FOBT must be done annually.
- How to collect a stool sample for FOBT
- Lay toilet paper in toilet bowl as shown on the right
Reverse sitting position as shown below allows for stool sample to be collected on the toilet paper for the FOBT test.
Immunochemical FOBTs do not need dietary restriction. Individuals with positive FOBT will require colonoscopy. Individuals with negative FOBT are tested annually.
Colonoscopy
Colonoscopy is the gold standard for complete large bowel evaluation. The main disadvantages are its higher cost, the need for full bowel preparation and sedation. There is also a small risk associated with the bowel preparation. For high-risk patients e.g., individuals at risk of hereditary non-polyposis colorectal cancer, colonoscopy is the screening investigation of choice.
The main advantages are its high sensitivity and specificity and the long recommended screening interval of 10 years. The protective effect of colonoscopy is attributed to the ability to remove asymptomatic polyps before malignant transformation occurs.
Usually, bowel preparation takes 1 of 2 forms: high-volume (3-4 litres) polyethene glycol (PEG) or low-volume (90 ml) oral fleet. Oral fleet is contraindicated in patients with renal impairment due to its high phosphate content. For suitable patients, it is a more palatable option as it can be mixed with sweetened fluids. Patients taking oral fleet must be encouraged to drink plenty of water to decrease the likelihood of phosphate toxicity.
General advice to patients on bowel preparation for patients undergoing colonoscopy:
Oral medications which need to be stopped before colonoscopy:
- Iron supplements (one week before appointment)
- Anticoagulation medications e.g. aspirin, Ticlid or warfarin (five days before the appointment)
Patients should go on a low fibre diet 3 days before colonoscopy, and avoid:
- Fruits and vegetables including fresh fruit and vegetable juices
- Vegetable soup
- Red meat
- Milk products
- Cereals and grains e.g. oats, bran, wheat, muesli, barley, nuts and beans
Foods allowed include:
- Simple carbohydrates (white rice, white bread, mee sua, bee hoon, kway teow, potatoes)
- Fish
- Plain coffee, tea, glucose, honey or clear soup
Colonoscopy is the gold standard for large bowel evaluation. The screening interval for colonoscopy is 10 years. Bowel preparation with low-volume oral fleet is feasible in the absence of contraindications.
Barium enema
A barium enema is an alternative to colonoscopy for large bowel evaluation. However, bowel preparation is still needed and in some studies, the false negative rate is as high as 50%. Furthermore, colonoscopy may still be needed to rule out suspicious lesions on the enema. There are currently no population screening studies using barium enemas.
CT Colonography/Virtual Colonoscopy
Virtual colonoscopy is a new radiologic technique used to generate images of the colon and rectal wall. Bowel preparation is still needed and like barium enema, colonoscopy may be needed for ruling out suspicious lesions and for therapeutic polypectomy.
A recent meta-analysis suggests that overall polyp detection rate is woefully inadequate, making this new technique unsuitable for population screening.