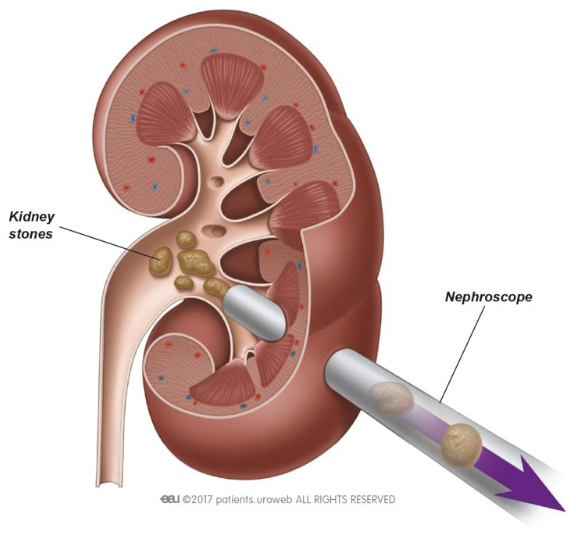
When the kidney stones are too large or complex for Extracorporeal Shock Wave Lithotripsy (ESWL), another treatment option is Percutaneous Nephrolithotomy (PCNL). This operation involves a small incision over the side where an instrument called a nephroscope is passed into the kidney and the stone is directly visualised and broken down with either an ultrasonic, pneumatic, or laser device. Depending on the size and type of stone, there is also an option of newer miniaturised access techniques such that the skin incision can be as small as possible.
After the operation, you will usually need to be warded overnight for observation. You may also have a temporary catheter placed in your side which can be removed in 1 - 2 days, which will be decided by the doctor.
What are the possible complications?
Some complications that may occur with PCNL include:
- Bleeding, in rare occasions needing blood transfusion
- Urinary tract infection
- Injury to the kidney and surrounding organs
Sometimes, more than one incision may be necessary to reach all the stones in the kidney. In some cases, there may still be remaining kidney stone fragments, which may require further procedures.
Advances in technology have allowed us to expand the treatments options for certain diseases. With better equipment, your kidney stones can be treated with a more personalised approach. For example, patients with many large kidney stones may require endoscopic combined intrarenal surgery (ECIRS), which involves concurrent PCNL and ureteroscopy, in order to achieve stone clearance in a minimal operative time.