Hand hygiene refers to the process of cleaning the hands by performing hand washing or through the use of alcohol-based hand rub solutions. In a healthcare setting, proper hand washing is the simplest way to reduce cross-transmission of microorganisms associated with infections which lead to increased length of stay, cost of care, and even mortality.
Despite this knowledge being imparted across all categories of healthcare staff, hand hygiene compliance rates have remained low. In multi-centre studies from 1981 to 1999, compliance to hand hygiene in ICUs has been observed to be less than 50%.1 In 2004, the WHO World Alliance for Patient Safety has initiated a global response in an effort to reduce healthcare-associated infections (HCAI), emphasizing the promotion of hand hygiene. Since then, various measurement tools and improvement efforts have been developed and implemented within and across countries.2
Measuring Hand Hygiene Compliance in NUH
Different institutions have their own ways of measuring hand hygiene compliance. They range from direct observation by trained observers, self-report by healthcare workers (HCWs), direct observation by patients, consumption of hygiene products and automated monitoring systems.3
The NUH audit process to measure hand hygiene compliance is very rigorous and it covers 33 wards and ICUs. The NUH Infection Prevention Team, hospital management and clinical stakeholders have been working together to refine its hand hygiene programme since 2006. It includes training and assessment of healthcare staff at all levels of seniority on the proper techniques and timing of hand washing. In addition, it uses measurement tools such as direct observation, measurement of product use and conducting surveys. The ultimate aim is to decrease the number of healthcare associated infections, especially that of MRSA (Methicillin-resistant Staphylococcus aureus).
The NUH Infection Prevention Team monitors staff hand hygiene compliance via covert observation. This means that the healthcare workers are not aware that they are being observed by an “undercover” auditor. This reduces bias because auditees tend to change their behaviour when they know that they are being audited (Hawthorne effect). Compliance is defined as the number of hand hygiene actions divided by the number of opportunities that require hand hygiene actions, multiplied by 100 and expressed as a percentage.
NUH adopts the World Health Organisation’s guidelines on the “Five Moments of Hand Hygiene”4
- Before touching a patient
- Before clean/aseptic procedure
- After body fluid exposure risk
- After touching a patient
- After touching patient surroundings
Training of healthcare staff on hand hygiene is done during orientation for new staff. Posters on hand washing techniques are put up at strategic locations. Yearly hand hygiene campaigns, like observance of Hand Hygiene Week, and video and poster competitions, have increased staff awareness of its importance. Hand Hygiene Assessment for staff is held every two years.
The chart below shows the quarterly compliance rate from 2018 (Figure 1). These overall rates have been encouraging as the hospital targets achieving >75% hand hygiene compliance. We have over 2000 observations hospital wide per quarter, conducted by trained auditors.
Figure 1: Hand Hygiene Compliance in NUH (ICUs and Wards)
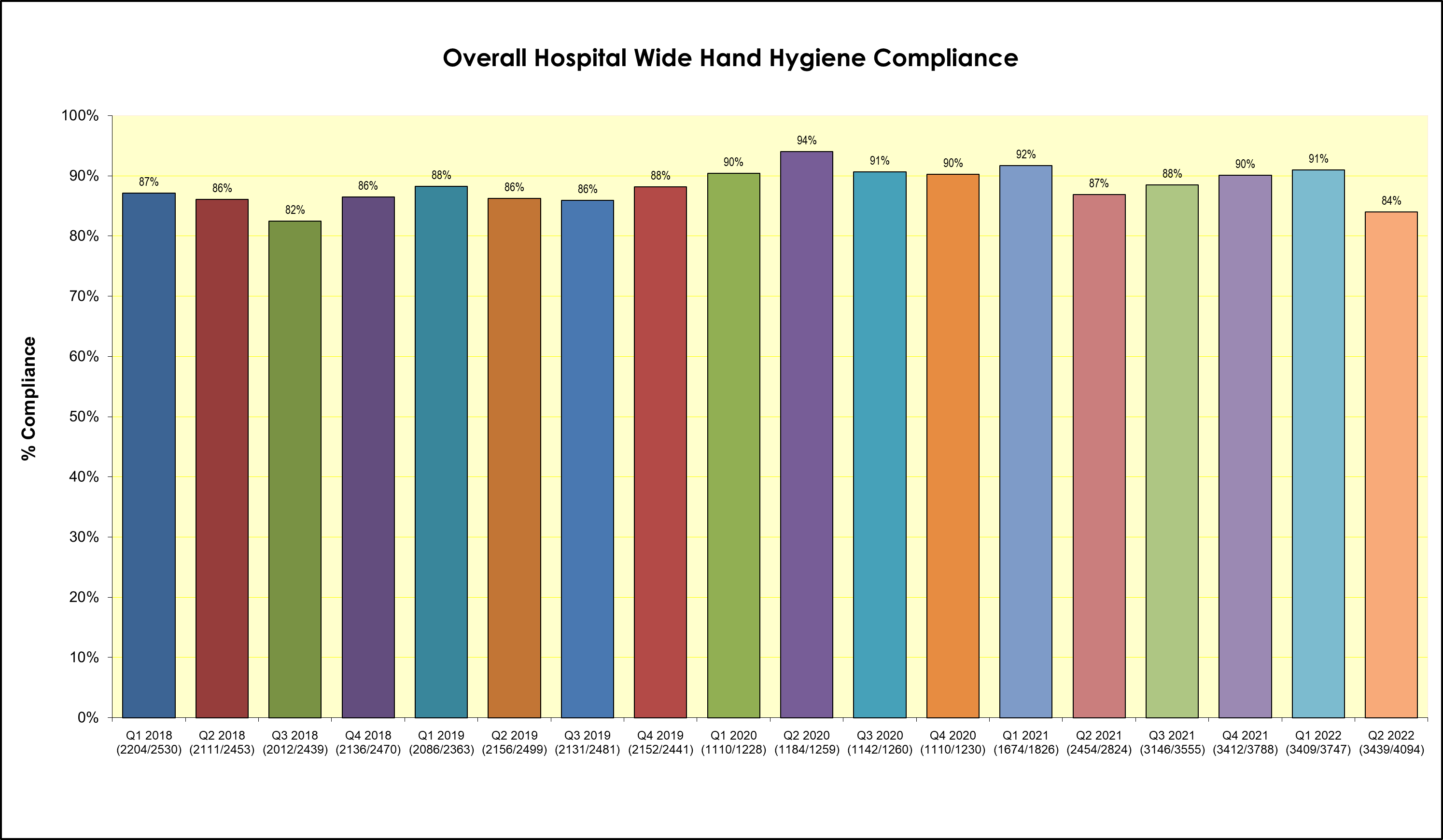
Source: NUH Infection Prevention
Information correct as of 19 July 2022.
Reference:
1. Pittet, D, “Improving Adherence to Hand Hygiene Practice: A Multidisciplinary Approach”, Emerging Infectious Diseases, Vol. 7, No. 2, March–April 2001
2. National Hand Hygiene: NHS Campaign Audit Report, 2007 http://www.documents.hps.scot.nhs.uk/hai/infection-control/national-hand-hygiene-campaign/audit-report.pdf, accessed on 20 May 2010
3. Measuring Hand Hygiene Adherence: Overcoming the Challenges http://www.jointcommission.org/NR/rdonlyres/68B9CB2F-789F-49DB-9E3F-2FB387666BCC/0/hh_monograph.pdf, accessed on 20 May 2010
4. “First Global Safety Challenge: Clean Care is Safer Care”, 2009, WHO Guidelines on Hand Hygiene in Health Care