 Subscribe and ensure you don't miss the next issue!
Subscribe and ensure you don't miss the next issue!
One in six pregnancies is affected by gestational diabetes mellitus (GDM) — a condition that temporarily raises blood sugar during pregnancy but can cast a long shadow over a woman’s health. The rate is higher in Singapore, with one in five expectant mothers developing the condition. What many don’t know is that GDM significantly increases the risk of developing type 2 diabetes later in life, with half of affected women developing it within a decade.
To help women safeguard their health beyond pregnancy, the National University Hospital (NUH) has launched a dedicated postpartum gestational diabetes service — a holistic, multidisciplinary programme that follows them from diagnosis through the postpartum years. It brings together specialists from obstetrics, endocrinology, and dietetics with close coordination between hospital and community care. Its goal is to close a critical gap in women’s health by tackling GDM and preventing diabetes before it develops.
The hidden risk after pregnancy
Women who develop gestational diabetes face a stark reality: their lifetime risk of type 2 diabetes increases by up to 70 per cent, with the danger peaking three to six years after childbirth. Despite these alarming statistics, most of them in Singapore see their care taper off after the standard six-week post-delivery glucose test, leaving early warning signs of poor blood sugar control undetected.
“GDM doesn’t end at delivery,” explains Dr Eng Pei Chia, Consultant, Division of Endocrinology, Department of Medicine, NUH, who leads the postpartum service. “Although many women with GDM are relatively young, their long-term risks are real. Women with GDM face increased lifetime risks of diabetes, heart disease, and fatty liver,”
A new model of continuous care
Since October 2023, NUH’s new postpartum service has supported nearly 400 mothers through a comprehensive and coordinated pathway.
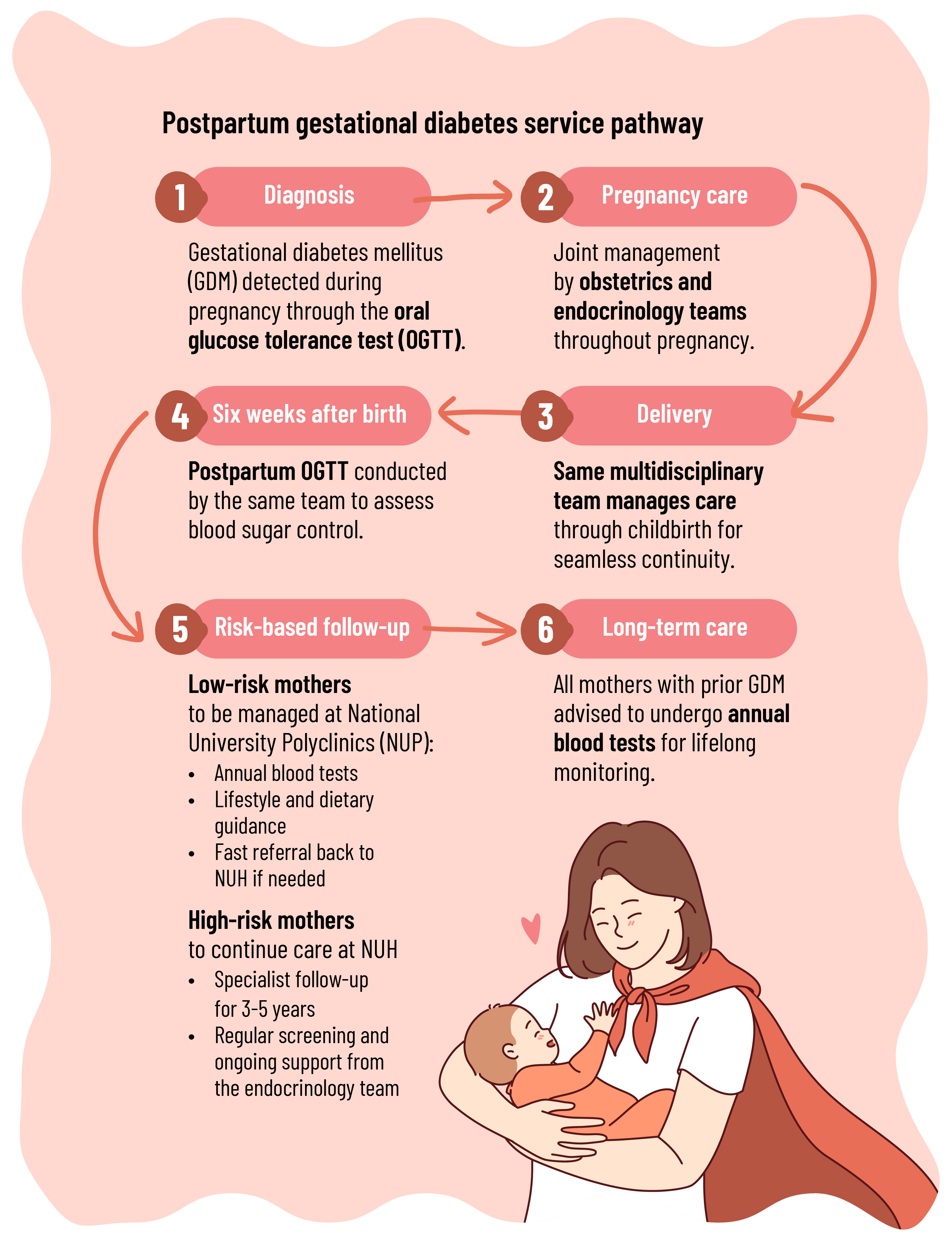
Supporting mothers beyond delivery
Through the new service, every mother with gestational diabetes receives continued support that extends beyond the delivery room. An experienced team of endocrinologists, obstetricians, and dietitians will work closely with each mother to restore their metabolic health and confidence to manage long-term wellness. The care goes beyond routine check-ups and monitoring. They receive practical, personalised guidance on diet, exercise, and sustainable lifestyle habits that lower their future diabetes risk.
For 40-year-old Mdm Cheryl Goh, being diagnosed with GDM during her second pregnancy came as a shock.
“I was in total disbelief. I even went back to retake my oral glucose tolerance test because I just couldn’t imagine I would have gestational diabetes, especially when I didn’t have it for my first pregnancy,” she recalls.
With the support of her healthcare team, Mdm Goh learned to include more slow-release carbohydrates into her meals, reduced refined sugar and incorporated light exercise such as brisk walking and weight training despite the challenges that come with motherhood. “The hardest part was staying consistent with two young children. Having a supportive healthcare team checking in and explaining my condition made it easier and less overwhelming,” she says.
Such follow-up proves essential, as about 40 per cent of mothers in the NUH programme continue to experience poor blood sugar control after delivery. Regular monitoring helps identify those at higher risk early and keeps them engaged in long-term care.
Protecting health across generations
The service’s impact extends beyond individual mothers. Adjunct Associate Professor Khoo Chin Meng, Head and Senior Consultant, Division of Endocrinology, Department of Medicine, NUH, emphasises the broader benefits: “By supporting women to make sustainable lifestyle changes through personalised routines, diet, and exercise, we can help them maintain good health and stay diabetes-free for as long as possible. This isn’t just about the mothers, but also about protecting their families and future generations.”
“With global rates of GDM rising by more than 30 per cent in the past two decades, it is important that we prioritise women’s health after birth,” adds Dr Eng. “When we provide sustained postpartum care for mothers, their children benefit too — through healthier homes and a reduced risk of diabetes across generations.”
Like this article? Simply subscribe to make sure you don't miss the next issue of EnvisioningHealth!





















