For short-duration, gentle exercises like a slow walk (less than 30 minutes), you may not need any additional preparation apart from bringing along some quick-acting carbohydrates to rescue hypoglycaemia.
However, the risk of hypoglycaemia during exercise increases with
- Longer durations of exercise (more than 30 minutes)
- More intense activities (e,g., cycling, running, prolonged hiking)
Here are FIVE general precautions to prevent hypoglycaemia during and after exercise.
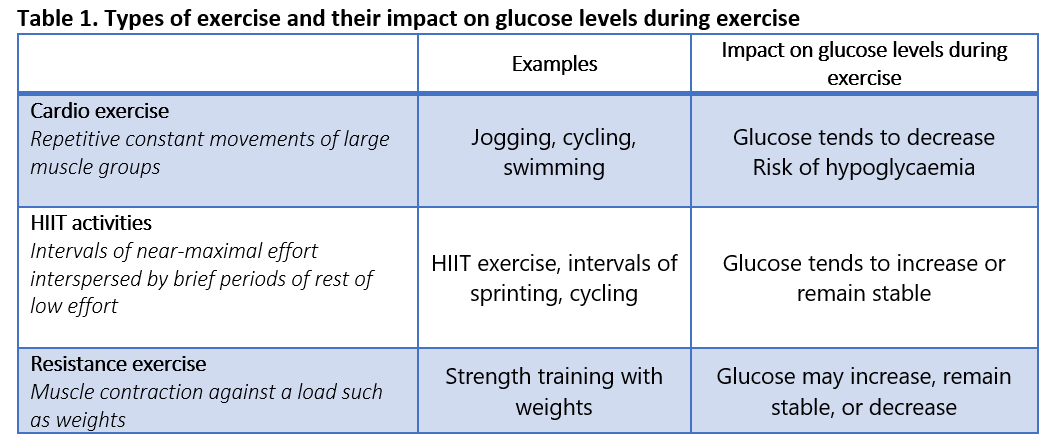
These precautions are primarily for cardio exercises but can also be applied to other types of exercise where glucose drops have been observed while exercising.

Before a planned exercise session
1. Prepare in advance by reducing the amount of active insulin in your body during the time of exercise
| Meal-Time Insulin | If exercising within three hours after a meal, reduce your meal-time insulin dose by 50% for that meal before the exercise.
If exercising more than three to four hours after a meal, consume a meal with low glycaemic index carbohydrates and administer your usual amount of meal-time insulin dose.
|
| Basal Insulin | For those using a basic insulin pump*, lower your basal insulin rates approximately 1.5 to 2 hours before you start cardio exercise.
If you are on basal insulin injections, consider reducing your basal insulin dose prior to exercise.
|
Consult your healthcare team for how to perform the above adjustment safely. For very long-duration exercises (four hours or more), additional preparation is necessary.
If you are on an advanced hybrid closed loop pumps, you should speak to your healthcare team as the above may not apply to you.
2. Prepare your exercise kit
- Ensure you have a glucometer with test strips and lancets, or if using a glucose sensor, bring along the reader/phone
- Carry quick-acting carbohydrates, such as glucose tablets, sweets or a tetrapack of sweet drink, for treating hypoglycaemia
- For exercise sessions longer than 30 minutes, prepare a carbohydrate snack to maintain glucose levels
3. Plan to exercise with a friend or family member who can assist you in case of hypoglycaemia
At the start of exercise: Start with a good pre-exercise glucose level
An ideal glucose level before starting exercise is between 7 to 10 mmol/L.
(These targets might be adjusted by your healthcare team based on your individual risk of hypoglycaemia.)
| Blood glucose level before cardio exercise (mmol/L) | Action to take before beginning cardio exercise | |
|---|
| < 4 | Avoid exercise, rescue hypoglycaemia. | |
| > 4 to 5 | Take 20g of carbohydrate* and recheck glucose before starting | |
| > 5 to 7 | Take 10g of carbohydrate* then start | |
| > 7 to 10 | Good to start | |
| >10 to 15 | OK to start, but exercise performance may be poorer | |
| >15 mmol/L | Check ketones and consider postponing exercise, especially if ketones are elevated | |
*Do not take additional insulin to cover these carbohydrates. Examples of 10g quick-acting carbohydrates:
- 200ml of isotonic drinks (not sugar free)
- 3 glucose tablets
- ½ packet of carbohydrate energy gels
- One small banana
During exercise
1. Carbohydrate replenishment
Aim to replenish carbohydrates every 30 to 60 minutes during cardio exercise. The amount required varies from 0.5 to 1 gram/kg body weight/hour of exercise, depending on the intensity. Higher intensity or failure to reduce insulin doses in advance will increase carbohydrate needs.
As a general guide, consume 15 to 30g of carbohydrates for every 30 minutes of moderate-intensity cardio exercise. For example, sipping on a bottle of isotonic drink during exercise can be effective to prevent hypoglycaemia (500ml of isotonic drink typically contains approximately 30g of carbohydrates).
2. Adding short bursts of high-intensity activity during cardio, such as intermittent sprinting while jogging, can help elevate blood glucose levels
3. If hypoglycaemia occurs, stop exercising immediately
4. Monitoring glucose levels using a continuous glucose sensor or flash glucose monitoring sensor.
If you are wearing a continuous glucose sensor or flash glucose monitoring sensor, monitor your glucose levels frequently during exercise.
Do remember that there is a lag time between the interstitial glucose read by the sensor and your actual blood glucose.
- We recommend that you start consuming carbohydrates when the sensor shows glucose levels falling below 7 mmol/L with a downward trend
- If the sensor reading drops to 5 mmol/L or below with downward trend, stop exercising and consume carbohydrates to prevent hypoglycaemia
- If experiencing hypoglycaemia symptoms but your CGMS does not reflect this, perform a finger-prick glucose check for accuracy.
Immediately after exercise
If your blood glucose is moderately high post-exercise, refrain from administering correction insulin. Instead, continue monitoring your levels, as the elevation is often temporary.