 Subscribe and ensure you don't miss the next issue!
Subscribe and ensure you don't miss the next issue!
 | Globally, younger adults consistently report higher stress levels than older age groups. A 2023 survey by the American Psychological Association found that adults aged 18–34 reported significantly higher stress scores than those over 55. In Singapore, that pattern holds. According to the Ministry of Health’s National Population Health Survey 2023–2024, one in four young adults reported poor mental health, the highest proportion among all age groups surveyed.
What is less well understood is what sustained stress does to the body over time — often happening without any warning signs, and well before any diagnosis.
Assistant Professor Cyrus Ho, Senior Consultant, Department of Psychological Medicine, National University Hospital (NUH), sees these patterns regularly in clinical practice. Here, he discusses why young Singaporeans are burning out earlier, how to recognise the warning signs, and what the evidence suggests about long-term consequences. |
SECTION 1: DETECTION
1 | Why does exhaustion feel so normal among people in their 20s and 30s today?
Modern life places continuous cognitive and psychological demands on people with very little structural recovery time. Social media amplifies comparison, creating a persistent sense of falling behind. Constant notifications keep the brain in a state of low-grade alertness — what might be described as always-on — making genuine disengagement difficult.
Lifestyle factors compound this. Later bedtimes, longer screen exposure, and poorer sleep quality reduce the body’s capacity to recover. Gradually, fatigue stops feeling like a signal and starts feeling like the baseline. |
2 | How can someone tell normal tiredness apart from something worth checking?
Temporary tiredness after a demanding period is pretty normal. But persistent fatigue that does not resolve with rest is different. Indicators worth taking seriously include ongoing exhaustion despite adequate sleep, difficulty concentrating, or physical symptoms such as unexplained weight changes, appetite disruption, or digestive problems. When several of these occur together and continue, a consultation is warranted. |
3 | What early warning signs should people watch for?
Warning signs span both the psychological and physical. They include poor or unrestorative sleep, persistent fatigue, frequent minor illnesses, increased irritability, and difficulty concentrating. Some people notice more rumination (feeling mentally stuck) or a gradual loss of motivation or interest in activities they previously enjoyed.
If these changes persist or begin affecting daily functioning — work performance, relationships, the ability to enjoy ordinary life — it may be time to seek support. |
SECTION 2: UNDERSTANDING
4 | What do people typically misunderstand about stress and burnout?
People respond to stress very differently. Some treat burnout as inevitable and keep pushing despite clear indicators. Others become so stress-sensitive that they try to avoid any pressure. Neither is the goal!
What matters is self-awareness: knowing when effort is sustainable and when recovery is overdue. Attitudes toward rest vary widely — some view taking breaks as a sign of weakness; others prioritise protecting their wellbeing above all else. The most important thing is being able to adjust to one’s own capacity and circumstances at different points in life. |
5 | Is it common to see people who appear successful but are quietly burning out?
Yes. In clinic, patients who appear outwardly high-functioning often present with subtle but telling signs. Some report cognitive concerns: difficulty multitasking, increased forgetfulness, or persistent brain fog. Others describe sleep difficulties: trouble falling asleep or waking unrefreshed despite adequate hours in bed.
Stress also manifests physically. Patients may present with headaches, abdominal discomfort, dizziness, or dry eyes despite unremarkable medical tests. Emotional symptoms — irritability, reduced stress tolerance, anxiety — are equally common. These presentations often look different on the surface but reflect the same underlying strain. |
6 | How does chronic stress affect the heart, metabolism, and immune system — even in someone who looks healthy?
Persistent stress activates the body’s stress response system in ways that compound over time. Cardiovascular effects include a subtle but sustained elevation in heart rate and blood pressure, alongside reduced heart rate variability — a marker of how well the body balances stress and recovery. These changes can occur even in physically active individuals.
Metabolically, prolonged stress hormone exposure, particularly cortisol, can promote insulin resistance, affect energy regulation and contribute to central weight gain. Immune function is also affected: while acute stress can temporarily stimulate immune activity, chronic stress disrupts immune regulation, increasing susceptibility to infection and sustaining a state of low-grade inflammation.
These processes occur at hormonal and cellular levels, meaning they are not visible in day-to-day appearance, which is part of why they go unrecognised. |
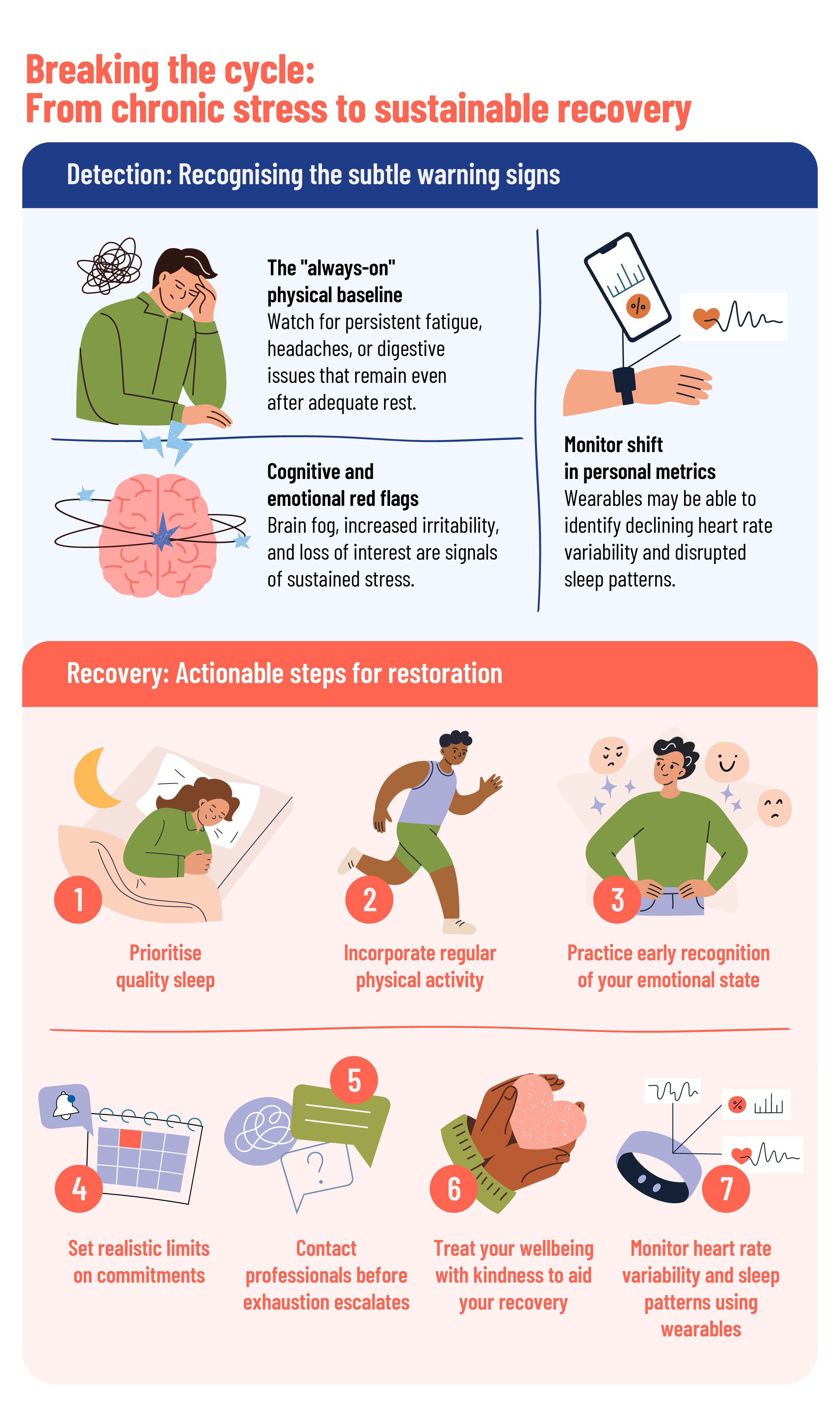
Warning signs to watch for and practical steps you can take.
SECTION 3: CONSEQUENCES
7 | What might happen if chronic stress goes unaddressed into midlife?
The downstream effects are well-documented. Prolonged stress exposure is associated with increased risk of cardiometabolic conditions — hypertension, insulin resistance, type 2 diabetes — as well as higher rates of anxiety, depression, and stress-related disorders. Cognitive effects, including difficulties paying attention and reduced mental stamina, can affect work performance and relationships. What concerns clinicians is not just the severity of these outcomes, but also how early they may appear when stress accumulates without intervention. |
SECTION 4: ACTION AND RECOVERY
8 | Are there simple health markers young adults can monitor?
Wearable devices and personal tracking can offer a useful window into stress and recovery. Metrics such as sleep duration, daily activity, step counts, and heart rate variability can reveal patterns. These are not diagnostic tools, but they can help individuals notice when something has shifted and prompt earlier action. |
9 | If someone feels overwhelmed, what practical steps actually help?
Sleep is the most evidence-backed starting point. Good sleep supports cognitive function, emotional regulation, metabolism, and immune health. In effect, it underlies almost every other system. Regular physical activity helps manage stress and improves sleep quality, but it does not substitute for adequate rest or offset chronic stress if the underlying causes remain unaddressed.
Early recognition is very important too. Checking in regularly with one’s physical and emotional state, setting realistic limits, and seeking support before exhaustion escalates are habits that reduce the risk of more serious outcomes. Practising self-compassion — treating one’s own wellbeing with the same care one would offer a close friend — is not a soft prescription. It has practical consequences for how the body recovers. |
Like this article? Simply subscribe to make sure you don't miss the next issue of EnvisioningHealth!






















