Subscribe and ensure you don't miss the next issue!
Subscribe and ensure you don't miss the next issue!
When 66-year-old Kiki Law (not her real name) noticed small blisters around her lips, she thought little of them. Perhaps a mild allergy, she figured. By the next day, pain shot from her neck to her head, and she could barely hear on one side. The diagnosis came as a surprise: shingles — a reactivation of the chickenpox virus she had as a child.
For 78-year-old Linda Giam, it began as a tingling sensation on her leg and a rough patch of skin which looked like a rash. Within hours, a line of blisters appeared. “Although I developed a line of small blisters, I didn’t feel any pain,” she recalls, “I didn’t know about shingles before this and didn’t know anyone who had it.”
These stories are not uncommon. Each year, an estimated 30,000 people in Singapore develop shingles, a condition that mostly affects older adults. Yet, many remain unaware of its potentially serious consequences.
“Many patients mistake the early signs for minor skin irritation or allergies,” says Professor Tan Huay Cheem, Senior Consultant, Department of Cardiology, National University Heart Centre, Singapore. “By the time the rash appears, the infection is already well underway. And what many don’t realise is that shingles can sometimes affect more than the skin — it can also raise the risk of heart attack and stroke.”
What exactly is shingles?
Shingles, or herpes zoster, stems from the varicella-zoster virus — the same culprit behind chickenpox. After a person recovers from chickenpox, the virus does not leave the body. Instead, it lies dormant in nerve cells for decades. When the immune system weakens with age or illness, the virus can reactivate, travelling along the nerves to the skin and causing a painful rash.
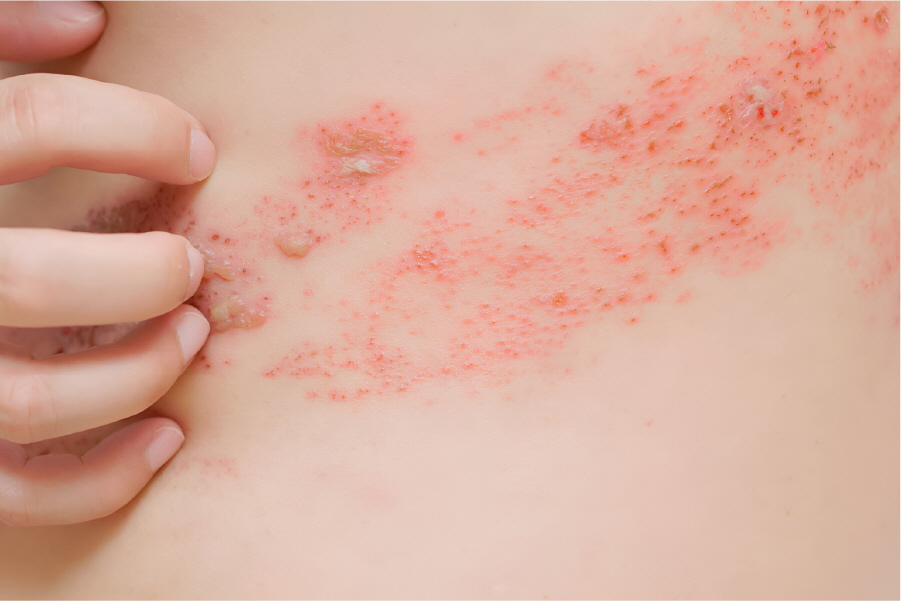
Early symptoms may appear days before the rash does. Some experience tingling, burning or sharp, needle-like pain on one side of the body or face. The rash then appears as small clusters of fluid-filled blisters, often forming a stripe or band. Over the next week or two, these blisters crust and heal, though discomfort can persist. In some cases, fever, fatigue and headaches accompany the rash.
Prompt treatment can reduce the severity and duration of symptoms. Antiviral medication is most effective when started within three days of the shingles rash appearing, which helps to limit viral activity and prevent complications. Pain relief and topical creams may also be prescribed to ease discomfort while the skin heals.
When shingles affects more than the skin
While most recover fully, some may develop postherpetic neuralgia — a condition causing persistent nerve pain that lingers for months or even years after the rash has healed. The pain, described as burning or stabbing, can disrupt sleep and daily activities. Shingles that occurs near the eyes or ears can also lead to complications such as vision or hearing loss, facial paralysis, or inflammation of the brain.
“Shingles is more common in those above 50, and the risk rises as the body’s immune response declines with age,” explains Prof Tan. “It can also occur in people with weakened immunity, such as those with diabetes, cancer or who are on immunosuppressive medications.”
More recently, research has shown that shingles can affect heart health. The infection triggers a systemic inflammatory response that can injure blood vessels and disrupt circulation, raising cardiovascular risks significantly. Within the first week of a shingles episode, the risk of heart attack increases by about 68 per cent, while the risk of stroke jumps by 78 per cent within a month. These elevated risks can persist for up to a year, with persistent pain and psychological stress further straining the cardiovascular system through blood pressure fluctuations.
“The virus can directly or indirectly damage the heart muscle, potentially leading to inflammation or heart failure in severe cases,” Prof Tan warns. "For older adults or those with pre-existing heart disease, shingles can pose a serious but often overlooked threat.”
A common misconception is that shingles only occurs in people who once had chickenpox. While that is true — the virus reactivates from a past infection — Prof Tan notes that even those vaccinated against chickenpox can still develop shingles later in life. “The virus, whether from natural infection or vaccination, remains in the body. It can reactivate when your immune defences weaken,” he explains.
Shingles can be prevented
As shingles has no cure, prevention remains the best safeguard especially for older adults and those with chronic illnesses. Vaccination significantly reduces the likelihood of developing shingles and its complications, from persistent nerve pain to life-threatening cardiovascular events.
In Singapore, the Shingrix vaccine is the only shingles vaccine approved by the Health Sciences Authority. It is a recombinant vaccine, meaning it contains a purified viral protein rather than a live virus, making it safe even for those with weakened immune systems. Clinical studies show over 90 per cent effectiveness in preventing shingles in adults over 50, with protection remaining strong for at least a decade. The two-dose regimen, administered two to six months apart, provides comprehensive coverage.
The Ministry of Health (MOH) now subsidises up to 75 per cent of vaccination costs for eligible citizens and permanent residents, bringing expenses down to approximately S$75 to S$300 per course for Singaporeans. From 2026, MediSave can be used to further offset vaccination costs.
Even those who have had shingles are advised to get vaccinated, as reccurrence affects up to 10 per cent of cases. “Having shingles once does not guarantee lifetime immunity,” notes Prof Tan. “Vaccination is highly effective in boosting the body’s immunity and providing long-term protection against shingles.”
Like this article? Simply subscribe to make sure you don't miss the next issue of EnvisioningHealth!