Subscribe and ensure you don't miss the next issue!
Subscribe and ensure you don't miss the next issue!
For nursing student Gwendolyn Lye, breathlessness arrived abruptly and alarmingly. A high fever and shortness of breath quickly escalated into heart failure, leaving the 22-year-old fighting for her life. For Nathan Tan1, dancing had always been central to his identity — until a severe pneumonia infection landed the 30-year-old in intensive care, where machines took over his failing lungs.
Both were critically ill and placed on extracorporeal membrane oxygenation (ECMO), a highly specialised form of life support reserved for patients whose hearts or lungs can no longer function on their own. Through the coordinated efforts of doctors, nurses, and physiotherapists at the National University Hospital (NUH) and the National University Heart Centre, Singapore (NUHCS), both patients were brought back from the brink of no possible survival. Their recoveries are also a testimony to how the team is advancing rehabilitation — including the use of awake ECMO — to give critically ill patients a better chance at faster recovery.
Preserving strength during life support
ECMO is used only when conventional treatments no longer work. By diverting blood through an external circuit that adds oxygen and removes carbon dioxide before returning it to the body, the system takes over the function of the heart and lungs, allowing them to rest and recover. Patients are often kept under deep sedation during this process, sometimes for weeks.
However, prolonged sedation in the intensive care unit (ICU) leaves patients highly vulnerable to ICU-acquired weakness — a rapid and profound loss of muscle mass. Studies have shown that critically ill patients can lose up to a quarter of their muscle mass within just four days in the ICU, and as much as half within a week. This can lead to severe weakness and lasting consequences: longer hospital stays, higher mortality and a diminished quality of life even after discharge.
To address this, the team at NUH and NUHCS introduced the use of awake ECMO, where selected patients are kept conscious and supported with careful airway management, pain control and close monitoring. This allows physiotherapists and nurses to begin gentle rehabilitation exercises early, which includes assisted stretching, mobility drills and later, simple strengthening exercises.
“By assisting patients with targeted movements while on awake ECMO, we help them return to physical function sooner, which shortens their recovery time,” says Dr Geetha Kayambu, Principal Physiotherapist and Research Director, Department of Rehabilitation, NUH. “It can prevent or mitigate ICU-acquired weakness, which can be debilitating and is one of the biggest challenges for patients on life support.”
Adjunct Associate Professor Prof K.R. Ramanathan, Senior Consultant, Cardiothoracic ICU, Department of Cardiac, Thoracic and Vascular Surgery, NUHCS, adds: “With awake ECMO patients, they can communicate better with the medical staff for more favourable outcomes, as well as partake in the rehabilitation process within a few days. It enhances their recovery, and they leave the ICU much earlier.”
Adj A/Prof Ramanathan also stresses that awake ECMO is not suitable for every patient, as success depends on factors such as airway stability, severity of illness and whether the patient can tolerate life support while conscious. For some, traditional ECMO with sedation remains the safest approach.
Journeys of recovery
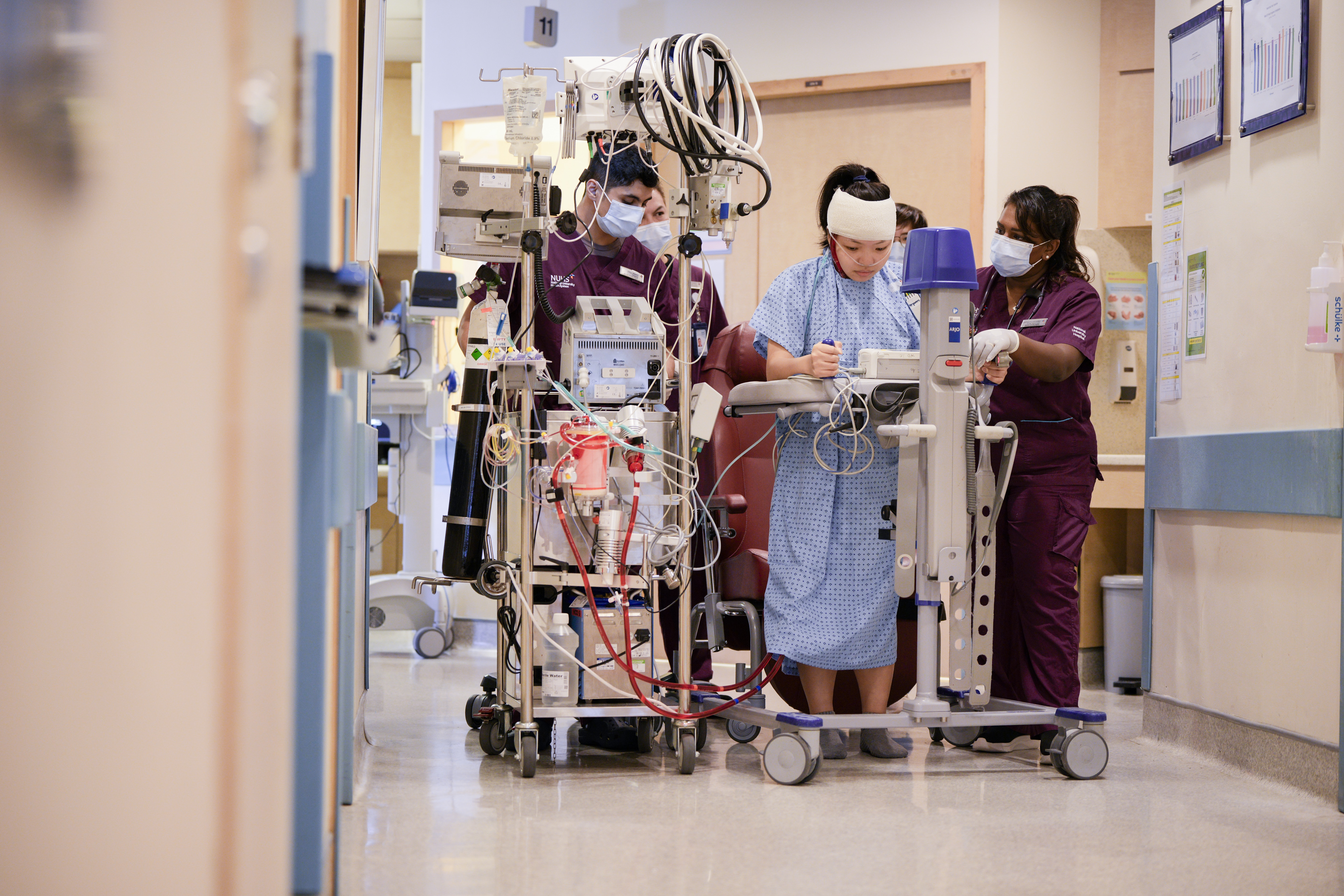
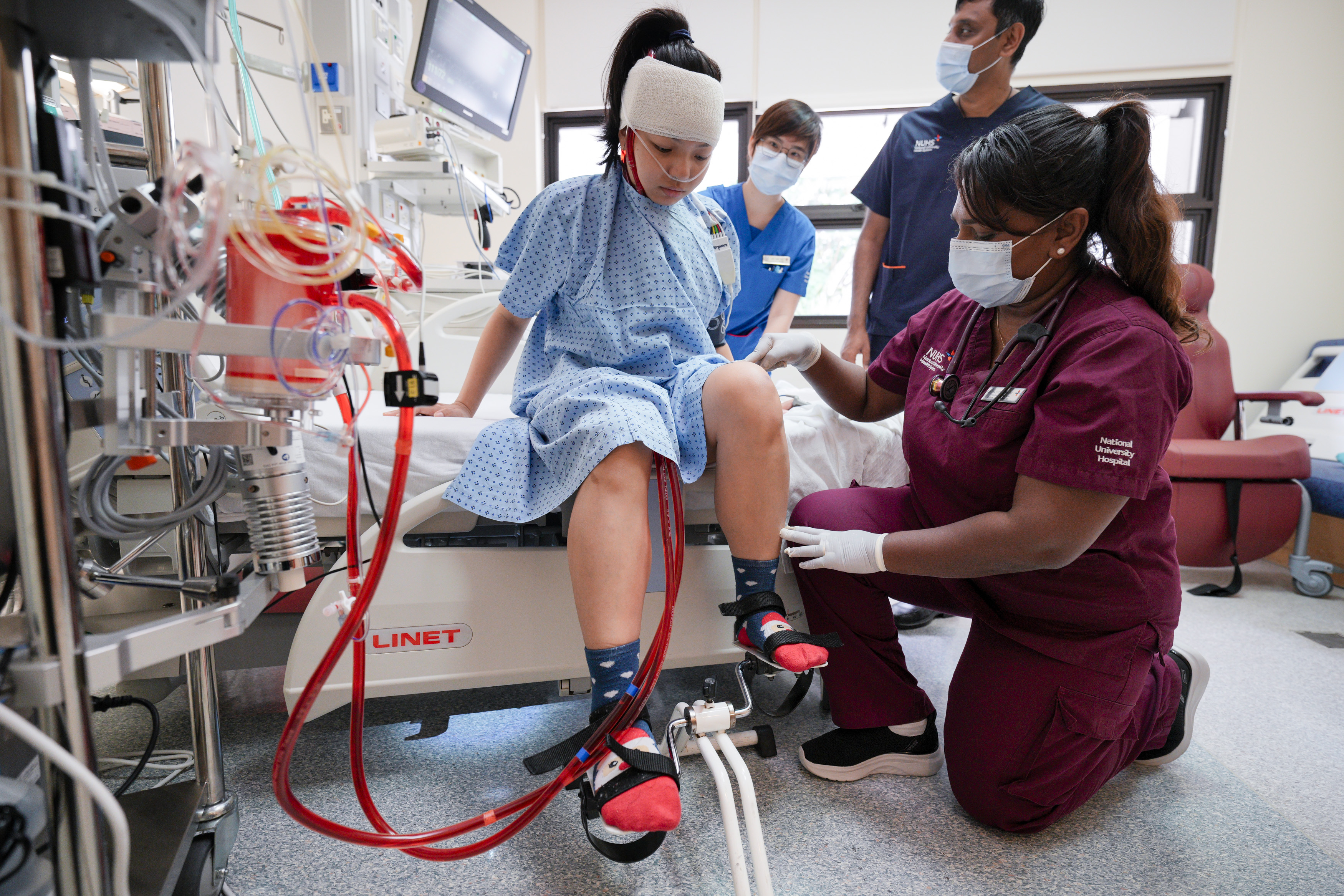
For Gwendolyn, awake ECMO meant she could remain conscious throughout the procedure. With her heart too weak to tolerate anaesthesia, the care team initiated life support while she was awake and immediately began gentle rehabilitation. Nurses and physiotherapists worked with her on stretching and mobility drills to slow muscle loss. Within four days, she was stable enough to be weaned off ECMO — half the typical duration. She has since returned to her nursing studies and resumed the active life she once feared she might lose.
Nathan’s recovery was more complex. He remained sedated during the initial weeks of ECMO. While he eventually recovered, his infection had caused gangrene, leading to a leg amputation. Rehabilitation began soon after surgery while he was still on ECMO. His first milestones were to sit up and participate in assisted exercises, before progressing to stationary cycling to rebuild strength. Knowing how important dance was to him, his physiotherapists incorporated dance-inspired movements into therapy, which helped him regain his confidence. Within a year, Nathan returned to the dance floor with a prosthetic leg.
“As much as the technology matters, it is the concerted effort of the multidisciplinary team that ensures patients recover well,” says Dr Kayambu. “Awake ECMO rehabilitation requires close coordination between the ICU, surgical teams, and therapists — it truly is a team effort to act swiftly and make the most of every opportunity to mobilise a critically ill patient.”
1 Individual’s name has been changed
Like this article? Simply subscribe to make sure you don't miss the next issue of EnvisioningHealth!