What Is Laser-Assisted Cataract Surgery?
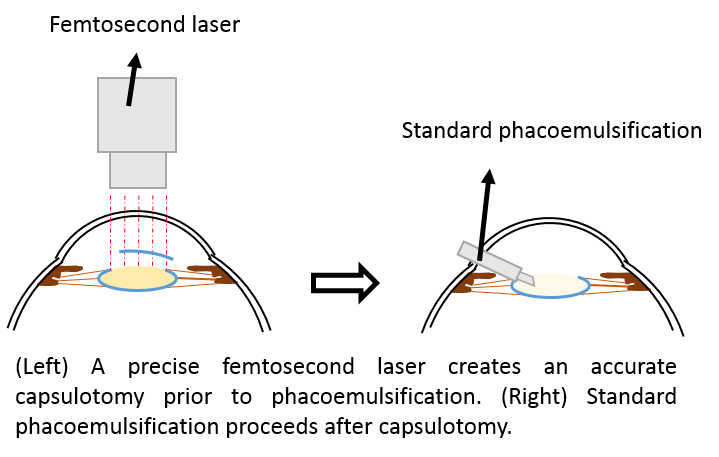
Femtosecond laser-assisted cataract surgery (FLACS) is the latest type of cataract extraction surgery, wherein a precise laser is used to replace certain steps of standard phacoemulsification. A laser creates an opening in the anterior lens capsule and softening the lens nucleus. It aims to reduce damage to the inner surface of the cornea while increasing precision of intraocular lens placement.
The laser procedure is first performed on a separate machine before the patient is transferred to the surgical bed for completion of the cataract surgery. The surgeon evaluate an individual's suitability for this procedure.
Would I See Better After FLACS Compared To Phacoemulsification?
There are many factors affecting the visual outcome after cataract surgery, such as the extent of spectacle power correction, inflammation degree and the wound healing process. It is advisable to discuss this with your eye doctor.
What Are The Additional Risks Of FLACS?
The complications associated with FLACS are similar to those of standard phacoemulsification, as evidenced by major clinical trials (Abell et al, 2014; Daya et al, 2014). The risks include anterior capsule tear and tags, increasing the likelihood of posterior capsule rupture. After the surgery, there may be swelling of the back of the eye (macula oedema) or elevated intraoperative pressure.
Who Should Consider FLACS?
FLACS may be beneficial for patients with less healthy corneas; however, it is not currently recommended as a standard procedure for all cataract surgeries (Day AC et al, 2016). The decision for FLACS should be discussed with your eye doctor.
References
Chen X, Xiao W, Ye S, et al. Efficacy and safety of femtosecond laser-assisted cataract surgery versus conventional phacoemulsification for cataract: a meta-analysis of randomized controlled trials. Sci Rep. 2015 Aug;13;5:13123.
Conrad-Hengerer I, Al Juburi M, Schultz T, et al. Corneal endothelial cell loss and corneal thickness in conventional compared with femtosecond laser-assisted cataract surgery: three-month follow-up. J Cataract Refract Surg. 2013 Sep;39(9):1307-13.